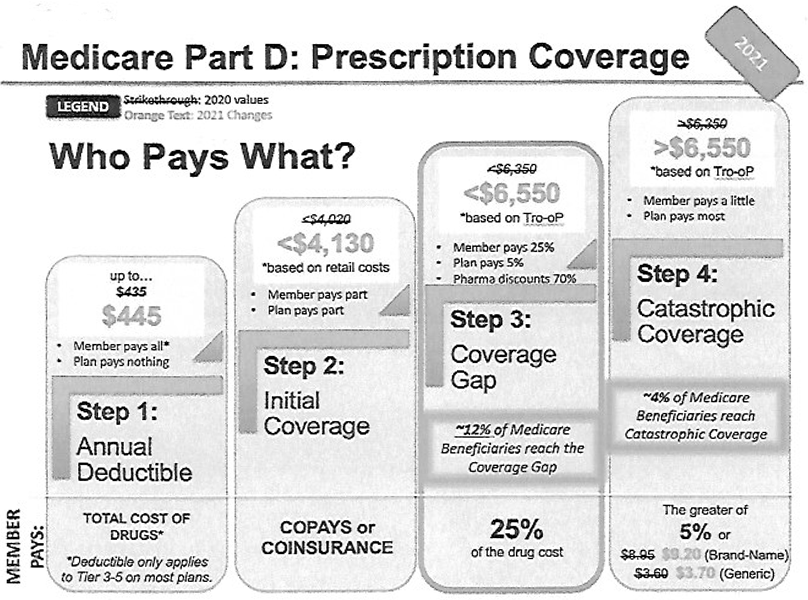
To be eligible for Medicare Part A and Part B, you must be a U.S. citizen or a permanent legal resident for at least five continuous years. Generally, Medicare is available for people age 65 or older, younger people with disabilities and people with End Stage Renal Disease (permanent kidney failure requiring dialysis or transplant), have Amyotrophic Lateral Sclerosis (ALS), also known as Lou Gehrig’s disease. Medicare has two parts, Part A (Hospital Insurance) and Part B (Medicare Insurance). You are eligible for premium-free Part A if you are age 65 or older and you or your spouse worked and paid Medicare taxes for at least 10 years. The standard monthly premium for Medicare Part B enrollees will be $148.50 for 2021. The annual deductible for all Medicare Part B beneficiaries is $203.00 in 2021.
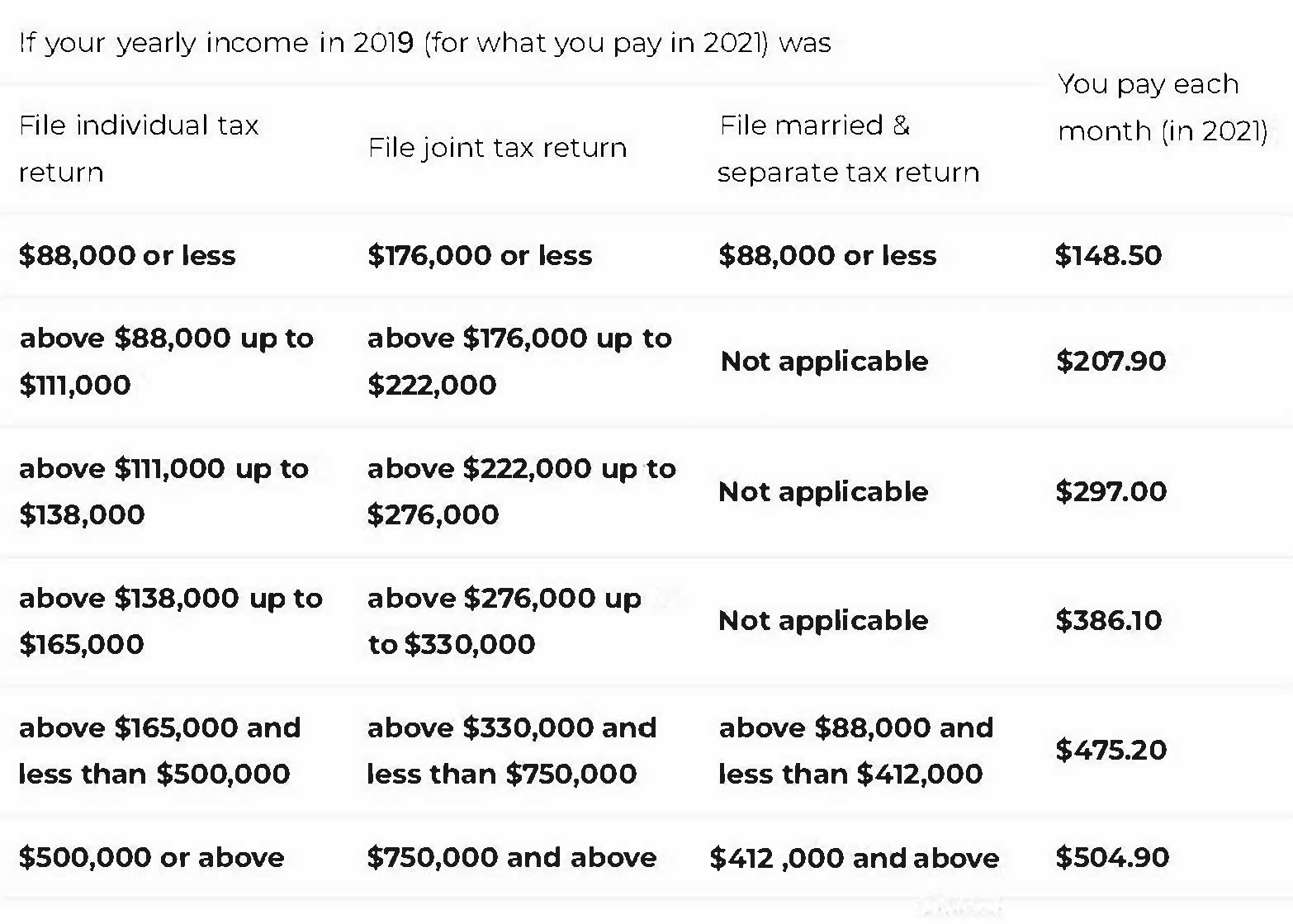
If you do not receive Social Security benefits:
If you are not receiving Social Security retirement benefits or Railroad Retirement benefits you will need to actively enroll in Medicare by calling the Social Security Administration at 800-772-1213 or online at socialsecurity.gov/medicareonly/.
If you already receive benefits from Social Security:
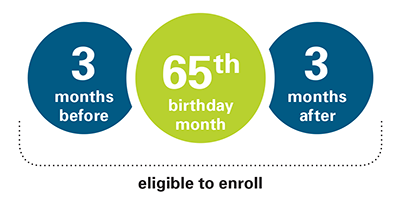
If you already get benefits from Social Security or the Railroad Retirement Board, you are automatically entitled to Medicare Part A (Hospital Insurance) and Part B (Medical Insurance) starting the first day of the month you turn age 65. You will not need to do anything to enroll. Your Medicare card will be mailed to you about 3 months before your 65th birthday. If your 65th birthday is February 20, 2010, your Medicare effective date would be February 1, 2010. (Note: if your birthday is on the 1st day of any month, Medicare Part A and Part B will be effective the 1st day of the prior month. For example, if your 65th birthday is February 1, 2010, your Medicare effective date would be January 1, 2010.)
If you are under age 65 and disabled:
If you are under age 65 and disabled, and have been entitled to disability benefits under Social Security or the Railroad Retirement Board for 24 months, you will be automatically entitled to Medicare Part A and Part B beginning the 25th month of disability benefit entitlement. You will not need to do anything to enroll in Medicare. Your Medicare card will be mailed to you about 3 months before your Medicare entitlement date. (Note: If you are under age 65 and have Lou Gehrig’s disease (ALS), you get your Medicare benefits the first month you get disability benefits from Social Security or the Railroad Retirement Board.) For more information about enrollment, call the Social Security Administration at 1-800-772-1213 or visit the Social Security website.
In general, Part A covers:
- • Inpatient care in a hospital
- • Skilled nursing facility care
- • Nursing home care (inpatient care in a skilled nursing facility that’s not custodial or long-term care)
- • Hospice care
- • Home health care
When you are admitted to a hospital or skilled nursing facility, Medicare Part A hospital insurance will cover the following for a certain amount of time:
- • A semi private room (two to four beds per room), or a private room if medically necessary
- • All meals, including special, medically required diets
- • Regular nursing services
- • special care units, such as intensive care and coronary care
- • Drugs, medical supplies, and appliances furnished by the facility, such as casts, splints, wheelchair; also, outpatient drugs and medical supplies if they permit you to leave the hospital sooner
- • Hospital lab tests, X-rays, and radiation treatment billed by the hospital
- • Operating and recovery room costs
- • Blood transfusions (you pay for the first three pints of blood, unless you arrange to have them replaced by an outside donation of blood to the hospital), and
- • Rehabilitation services, such as physical therapy, occupational therapy, and speech pathology, provided while you are in the hospital.
To find out if Medicare covers a service not on this list, visit www.medicare.gov/coverage, or call 1-800-MEDICARE (1-800-633-4227). TTY users should call 1-877-486-2048.
The main coverage options include:
- Original Medicare, which comprises: Medicare Part A – hospital insurance. Medicare Part B – outpatient coverage.
- Original Medicare, which comprises: Medicare Part A – hospital insurance. Medicare Part B – outpatient coverage.
- Medicare Advantage (Part C) A Medicare Advantage Plan (like an HMO or PPO) is another Medicare health plan choice you may have as part of Medicare. Medicare Advantage Plans, sometimes called “Part C” or “MA Plans,” are offered by private companies approved by Medicare. If you join a Medicare Advantage Plan, the plan will provide all of your Part A (Hospital Insurance) and Part B (Medical Insurance) coverage. Medicare Advantage Plans may offer extra coverage, such as vision, hearing, dental, and/or health and wellness programs. Most include Medicare prescription drug coverage (Part D).
- Medicare Advantage (Part C) A Medicare Advantage Plan (like an HMO or PPO) is another Medicare health plan choice you may have as part of Medicare. Medicare Advantage Plans, sometimes called “Part C” or “MA Plans,” are offered by private companies approved by Medicare. If you join a Medicare Advantage Plan, the plan will provide all of your Part A (Hospital Insurance) and Part B (Medical Insurance) coverage. Medicare Advantage Plans may offer extra coverage, such as vision, hearing, dental, and/or health and wellness programs. Most include Medicare prescription drug coverage (Part D).
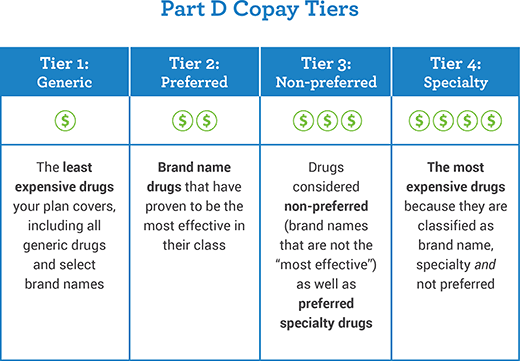
- Medicare Part D – prescription drug coverage.Medicare Part D is simply insurance for your medication needs. You pay a monthly premium to an insurance carrier for your Part D plan. In return, you use the insurance carrier’s network of pharmacies to purchase your prescription medications. … Your Part Dinsurance card will be separate from your Medigap plan.
Medigap – Medicare Supplement insurance. Medigap is extra health insurance that you buy from a private company to pay health care costs not covered by Original Medicare, such as co-payments, deductibles, and health care if you travel outside the U.S. Medigap policies don’t cover long-term care, dental care, vision care, hearing care, vision care, hearing aids, eyeglasses, and private -duty nursing. Most plans do not cover prescription drugs.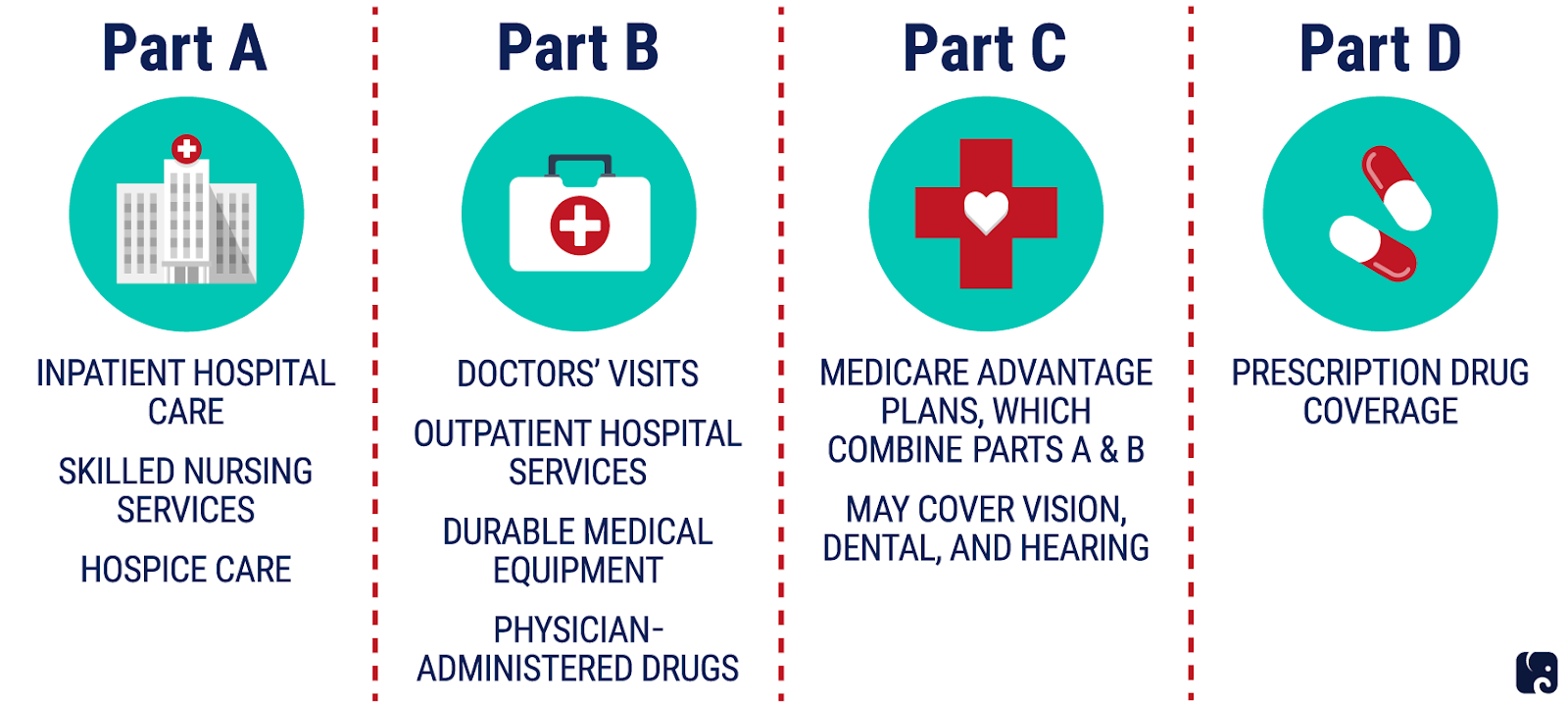
| Costs for Part A (Hospital): | What you pay in 2025: |
|---|---|
| Premium | $0 for most people (because they or a spouse paid Medicare taxes long enough while working – generally at least 10 years). If you get Medicare earlier than age 65, you won’t pay a Part A premium. This is sometimes called “premium-free Part A.” If you don’t qualify for premium-free Part A: You might be able to buy it. You’ll pay either $278 or $506 each month for Part A, depending on how long you or your spouse worked and paid Medicare taxes. Remember:
|
| Deductible | $1,600 for each inpatient hospital , before starts to pay. There’s no limit to the number of benefit periods you can have in a year. This means you may pay the deductible more than once in a year. |
| Inpatient stay |
|
| Skilled nursing facility stay |
|
| Home health care | $0 for covered home health care services. 20% of the for durable medical equipment (like wheelchairs, walkers, hospital beds, and other equipment) |
| Hospice care | $0 for covered hospice care services. You may also pay: |

Part B (Medical Insurance) costs
| Part B costs: | What you pay in 2023: |
|---|---|
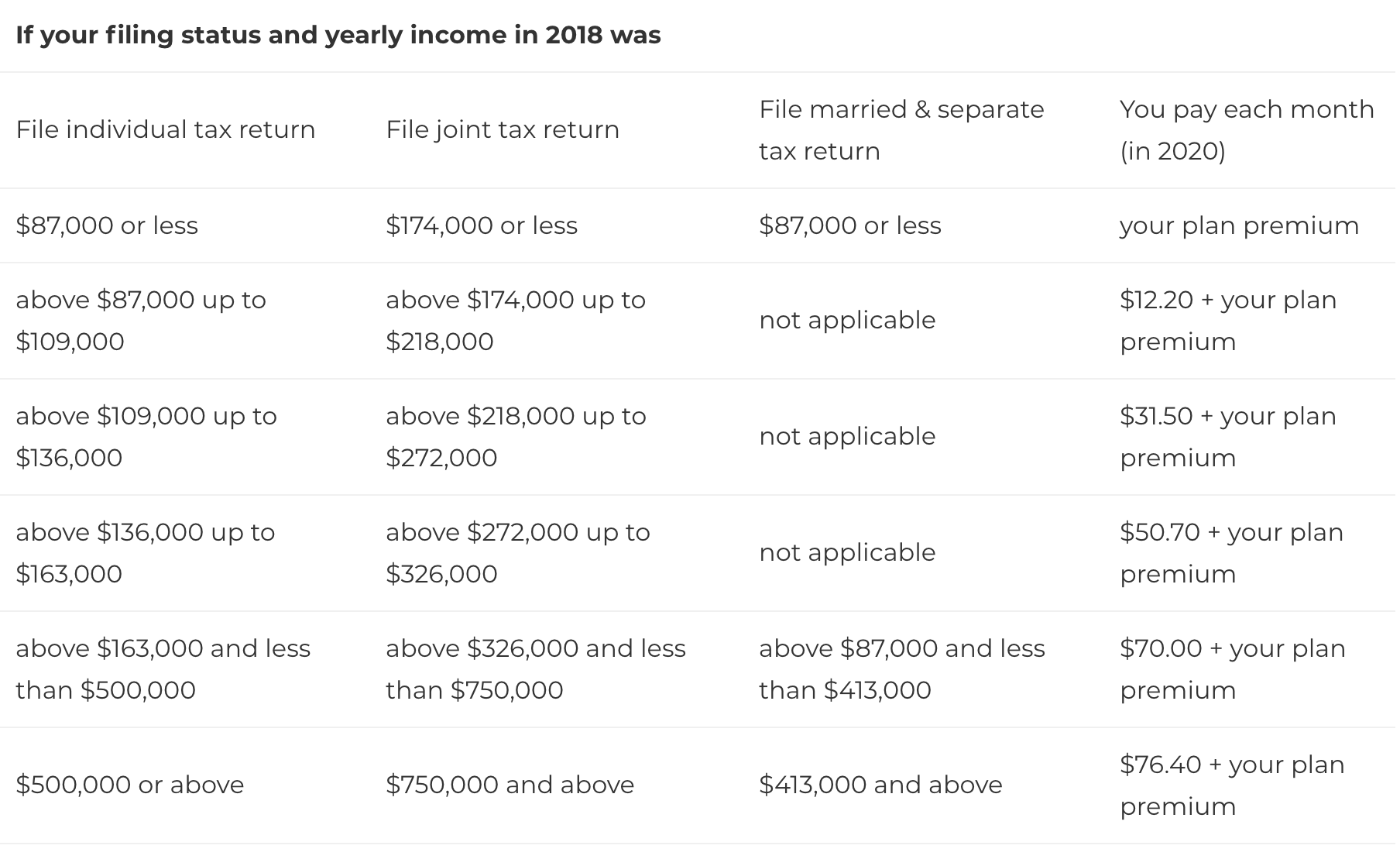
| Premium | $164.90 each month (or higher depending on your income). The amount can change each year. You’ll pay the premium each month, even if you don’t get any Part B-covered services. You might pay a monthly penalty if you don’t sign up for Part B when you’re first eligible for Medicare (usually when you turn 65). You’ll pay the penalty for as long as you have Part B. The penalty goes up the longer you wait to sign up. Find out how the Part B penalty works and how to avoid it. |
| Deductible | $226, before Original Medicare starts to pay. You pay this deductible once each year. |
| General costs for services (coinsurance) | Usually 20% of the cost for each Medicare-covered service or item after you’ve paid your deductible (and as long as your doctor or health care provider accepts the as full payment – called “accepting assignment”). Find out how assignment affects what you pay. |
| Clinical laboratory services | $0 for covered clinical laboratory services. |
| Home health care |
|
| Inpatient hospital care | 20% of the for most doctor services while you’re a hospital inpatient. |
| Outpatient mental health care |
|
| Partial hospitalization mental health care | After you meet the Part B deductible:
|
| Outpatient hospital care |
|
Costs for Part A (Hospital): What you pay in 2025:
Part A Premium
$0 for most people (because they paid Medicare taxes long enough while working – generally at least 10 years). This is sometimes called “premium-free Part A.” Do I qualify?
If you don’t qualify for a premium-free Part A, you might be able to buy it. In 2025, the premium is either $285 or $518 each month, depending on how long you or your spouse worked and paid Medicare taxes.
You also have to sign up for Part B to buy Part A.
If you don’t buy Part A when you’re first eligible for Medicare (usually when you turn 65), you might pay a penalty.
How much is the Part A penalty?
Part A Deductible
$1,676 for each time you’re admitted to the hospital per benefit period, before Original Medicare starts to pay. There’s no limit to the number of benefit periods you can have.
Inpatient stays (copayments)
Days 1-60: $0 after you pay your Part A deductible
Days 61-90: $419 each day
Days 91-150: $838 each day while using your 60 lifetime reserve days
After day 150: You pay all costs Costs for Part B (Medical Insurance)
Costs for Part B (Premium): What you pay in 2025:
Part B Premium
$185 each month (or higher depending on your income). The amount can change each year. You’ll pay the premium each month, even if you don’t get any Part B-covered services.
Who pays a higher premium because of income?
How do I pay my Part B premiums?
You might pay a penalty if you don’t sign up for Part B when you’re first eligible for Medicare (usually when you turn 65). Check when I should sign up for Part B.
How much is the Part B late enrollment penalty?
You’ll pay an extra 10% for each year you could have signed up for Part B, but didn’t.
This penalty is added to your monthly Part B premium. (You may also pay a higher premium depending on your income.)
It’s not a one-time late fee — you’ll pay the penalty for as long as you have Part B.
Generally, you won’t have to pay a penalty if you qualify for a Special Enrollment Period. To qualify, you (or your spouse) must still be working and you must have health coverage based on that job.
Example of the Part B penalty.
Part B Deductible
You’ll pay $257, before Original Medicare starts to pay. You pay this deductible once each year.
Costs for services (coinsurance) You’ll usually pay 20% of the cost for each Medicare-covered service or item after you’ve paid your deductible.
Skilled Nursing Facility Care
Medicare Part A (Hospital Insurance) covers skilled nursing facility care for a limited time (on a short-term basis) if you meet all of these conditions:
- You have Part A and have days left in your benefit period to use.
- You have a qualifying inpatient hospital stay.
- You enter the SNF within a short time (generally 30 days) of leaving the hospital.
- Your doctor or other health care provider has decided that you need daily skilled care (like intravenous fluids/medications or physical therapy). You must get the care from, or under the supervision of, skilled nursing or therapy staff.
- You get these skilled services in a Medicare-certified SNF.
- You need skilled services for one of these:An ongoing condition that was also treated during your qualifying inpatient hospital stay (even if it wasn’t the reason you were admitted to the hospital). A new condition that started while you were getting SNF care for the ongoing condition. You need skilled nursing care or therapy to improve or maintain your current condition, or to prevent or delay it from getting worse.
What’s a qualifying inpatient hospital stay? - A qualifying inpatient hospital stay means you’ve been a hospital inpatient for at least 3 days in a row (counting the day you were admitted as an inpatient, but not counting the day of your discharge). Medicare will only cover care you get in a SNF if you first have a “qualifying inpatient hospital stay.” What are some example situations?
- Time that you spend in a hospital as an outpatient before you’re admitted doesn’t count toward the 3-day qualifying inpatient hospital stay you need to get SNF benefits.
How do hospital observation services affect my SNF coverage?
You may not need a 3-day minimum inpatient hospital stay if your doctor participates in an Accountable Care Organization or another type of Medicare initiative approved for a “Skilled Nursing Facility 3-Day Rule Waiver.”
Always ask your doctor or hospital staff if Medicare will cover your SNF stay. Medicare Advantage Plans may also waive the 3-day minimum. Contact your plan for more information.
If you don’t have a 3-day qualifying inpatient hospital stay and you need care after your discharge from a hospital, ask if you can get care in other settings (like home health care) or if any other programs (like Medicaid or Veterans’ benefits) can cover your SNF care.
Your costs in Original Medicare
In each benefit period, you pay:
Days 1 – 20: $0. (Note: If you’re in a Medicare Advantage Plan, you may be charged copayments during the first 20 days. Check with your plan for more information.)
Days 21 – 100: $209.50 each day
Days 101 and beyond: All costs
Part A limits SNF coverage to 100 days in each benefit period.
Frequency of services
Your doctor or other health care provider may recommend you get services more often than Medicare covers. Or, they may recommend services that Medicare doesn’t cover. If this happens, you may have to pay some or all of the costs. Ask questions so you understand why your doctor is recommending certain services and if, or how much, Medicare will pay for them.
What it is
Skilled care is nursing and therapy care that can only be safely and effectively performed by, or under the supervision of, professionals or technical personnel. It’s health care given when you need skilled nursing or skilled therapy to treat, manage, and observe your condition, and evaluate your care.
Medicare-covered services in a skilled nursing facility include, but aren’t limited to:
- A semi-private room (a room you share with other patients)
- Meals
- Skilled nursing care
- Physical therapy (if needed to meet your health goal)
- Occupational therapy (if needed to meet your health goal)
- Speech-language pathology services (if they’re needed to meet your health goal)
- Medical social services
- Medications
- Medical supplies and equipment used in the facility
- Ambulance transportation (when other transportation endangers your health) to the nearest supplier of needed services that aren’t available at the SNF
- Dietary counseling
Things to know
Readmission to a hospital
If you’re in a SNF, there may be situations where you need to be readmitted to the hospital. If this happens, there’s no guarantee that a bed will be available for you at the same SNF if you need more skilled care after your hospital stay. Ask the SNF if it will hold a bed for you if you must go back to the hospital. Also, ask if there’s a cost to hold the bed for you.
After you leave the SNF, if you re-enter the same or another SNF within 30 days, you don’t need another 3-day qualifying hospital stay to get additional SNF benefits. This is also true if you stop getting skilled care while in the SNF and then start getting skilled care again within 30 days.
Refusing care
If you refuse your daily skilled care or therapy, you may lose your Medicare SNF coverage. If you have a condition that keeps you from getting skilled care (like if you get the flu), you may be able to continue to get Medicare coverage temporarily.
Stopping care or leaving
If you stop getting skilled care in the SNF, or leave the SNF altogether, your SNF coverage may be affected depending on how long your break in SNF care lasts. If you disagree with your discharge for any reason, you can appeal.
If your break in skilled care lasts more than 30 days, you need a new 3-day hospital stay to qualify for additional SNF care. The new hospital stay doesn’t need to be for the same condition that you were treated for during your previous stay.
If your break in skilled care lasts for at least 60 days in a row, this ends your current benefit period and renews your SNF benefits. This means that the maximum coverage available would be up to 100 days of SNF benefits.
You can appeal past hospital stays back to January 2009
If you’re a Medicare patient who was admitted to the hospital as an inpatient, and the hospital changed your status to “outpatient getting observation services,” you may be able to appeal the denial of Part A (Hospital Insurance) inpatient coverage that came from the change in your status. If your appeal is approved, Part A may cover the hospital and skilled nursing facility (SNF) services (if appealed) you got.
Get more information on how to file this type of appeal.
Medicare doesn’t cover everything. Some of the items and services Medicare doesn’t cover include:
- ✖ Long Term Care (also called custodial care)
- ✖ Most dental care
- ✖ Eye exams related to prescribing glasses
- ✖ Dentures
- ✖ Cosmetic surgery
- ✖ Hearing aids and exams for fitting them
- ✖ Routine foot care
Medicare does not cover Custodial Care, also referred to as long-term care. Part A coverage will help pay for short-term stays in skilled nursing facilities. As opposed to skilled nursing that is performed by licensed medical professionals, custodial care can be provided by non-licensed caregivers. Some Medicare Advantage Plans (Part C) offer extra benefits that Original Medicare doesn’t cover like limited custodial care.
Original Medicare (Part A and Part B) does not cover routine Dental or Vision care. There are certain circumstances under which Original Medicare may provide some coverage for dental or vision in case of an emergency setting or as part of surgery preparation. Medicare doesn’t cover eye exams for eyeglasses or contact lenses. Some Medicare Advantage Plans (Part C) offer extra benefits that Original Medicare doesn’t cover like dental and vision care. Medicare doesn’t cover hearing aids or exams for fitting hearing aids. You pay 100% for hearing aids and exams. Some Medicare Advantage Plans (Part C) offer extra benefits that Original Medicare doesn’t cover – hearing and exams for fitting them.
Medicare never covers Ambulette services. An Ambulette is a wheelchair-accessible van that provides non-emergency transportation. Medicare may cover scheduled, regular trips if the ambulance supplier receives a written order from your doctor ahead of time stating that transport is medically necessary. Original Medicare (Part A and Part B) generally does not cover transportation to get routine health care. However, it may cover non-emergency ambulance transportation to and from a health-care provider. Some Medicare Advantage Plans (Part C) offer extra benefits that Original Medicare doesn’t cover like transportation.
Medicare usually does not cover medical care you receive when traveling outside the U.S. and its territories. In limited situations, Medicare may pay for non-emergency inpatient services in a foreign hospital (and any connected provider and ambulance costs). Some Medicare Advantage Plans (Part C) offer extra benefits that Original Medicare doesn’t cover like emergency foreign coverage.
Medicare is an insurance program. Medical bills are paid from trust funds which those covered have paid into. It serves people over 65 primarily, whatever their income; and serves younger disabled people and dialysis patients. Patients pay part of costs through deductibles for hospital and other costs. Small monthly premiums are required for non-hospital coverage. Medicare is a federal program. It is basically the same everywhere in the United States and is run by the Centers for Medicare & Medicaid Services, an agency of the federal government.
Medicaid
Medicaid is an assistance program. It serves low-income people of every age. Patients usually pay no part of costs for covered medical expenses. A small co-payment is sometimes required. Medicaid is a federal-state program. It varies from state to state. It is run by state and local governments within federal guidelines.